- Book Now
-
-
Surgical
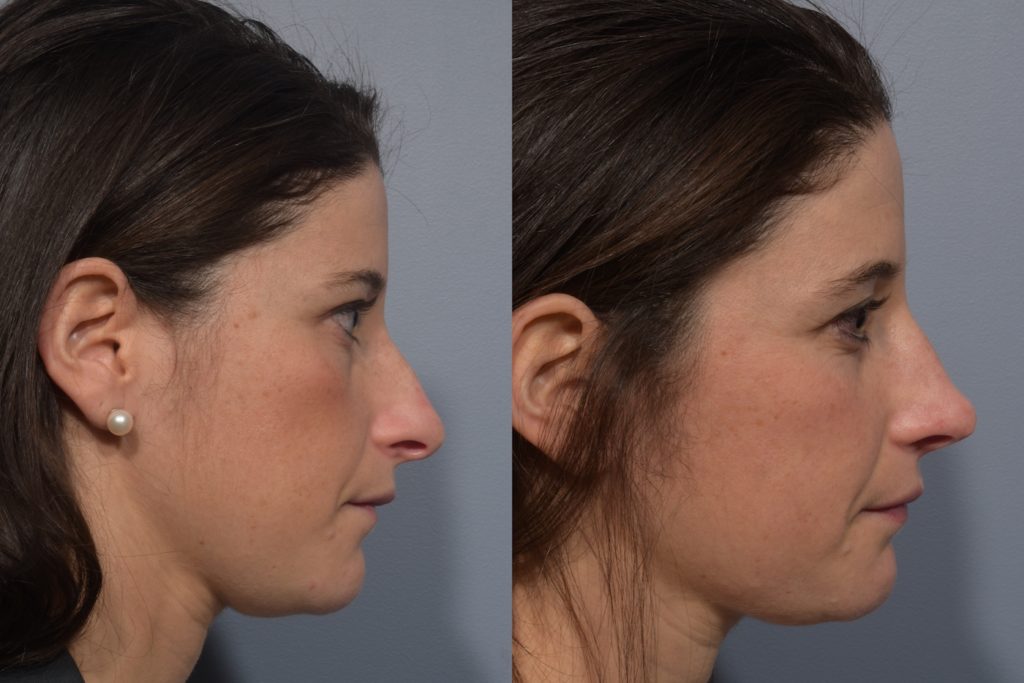
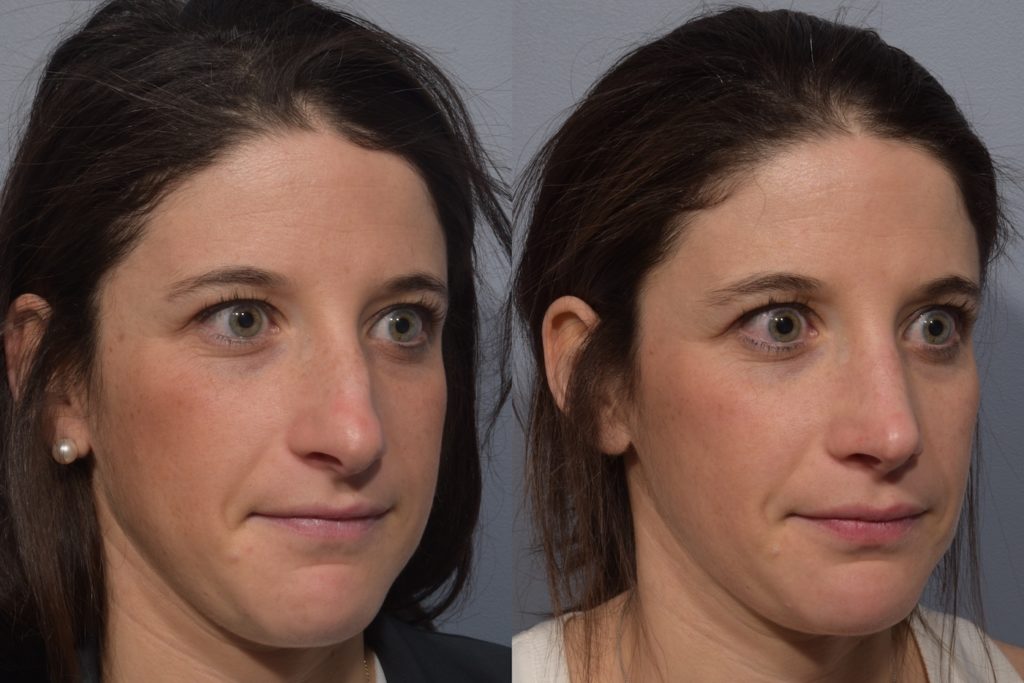
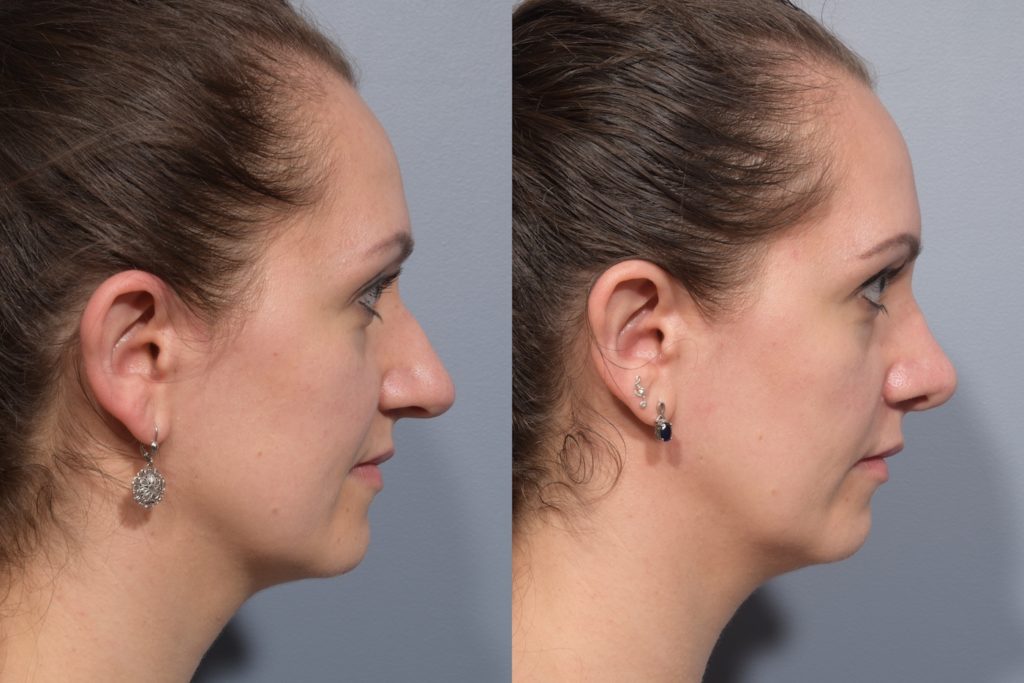
- Before & After
-
-
About Surgery
- For Women
- For Men
- Extreme Makeover
- Frequently Asked Questions & Reviews
-
-
-
-
Non-Surgical
-
-
Skin Tightening
- Ultherapy
- FaceTite
- Non-Surgical Facelift
- MyEllevate Neck Lift
- Nécolleté™
- View All
-
-
-
Body Sculpting
- Non-Surgical BBL
-
- Skincare
- Before & After
-
- All Treatments
-
-
Story & Staff
- Our Mission
- Our Staff
- Our Approach
- Meet Dr. Pearlman
-
- Before & After
- Contact
- Blog

Welcome to Pearlman Aesthetic Surgery for septoplasty in NYC on Park Avenue.
Septoplasty, or correcting a deviated septum, is usually performed from inside the nose by a closed, scarless, or endonasal approach. That means that Dr. Pearlman moves, scores, reshapes, or removes crooked cartilage and bone to correct the septum and improve functionality.
Breathe easier with functional nasal surgery.
Do you ever feel like one side of your nose is always stuffed up or blocked?
That may indicate you have a deviated septum, which is the most common cause of a continual nasal obstruction.
It can be uncomfortable and even change your sleep patterns. Some patients find they need to sleep with the blocked side down towards the pillow to allow the more open nostril to breathe. Sleeping with the blocked side up can mean trouble breathing and sleep issues.
The culprit is the septum: the wall between the two sides of the nose. It can become crooked, or “deviated” for any number of reasons. While some people can pinpoint an incident that pushed their septum out of shape, most of us just have no recollection of a cause. Maybe you fell on your nose as a child or perhaps your nose was traumatized during birth.
Either way, it turns out that many people have mildly deviated septums that cause no problems whatsoever. If there is no nasal blockage, obstruction or frequent sinusitis, then a mildly deviated septum doesn’t need to be fixed unless you are considering rhinoplasty.
Functional Nasal Surgery
More Information
Diagnosing a Deviated Septum
Fixing a Deviated Septum
Septoplasty vs. Rhinoplasty
Other Causes & Sinus Surgery
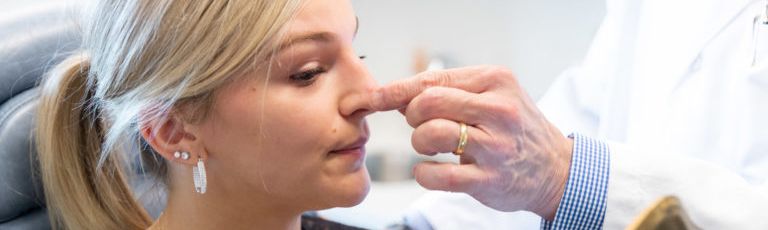
If you are finding you have trouble breathing either during the day or at night, with one side of your nose constantly feeling blocked, that can be fixed. First, we diagnose a deviated septum by a careful examination of the inside of the nose. Most nose surgeons will use a headlight and a small device called a nasal speculum to inspect the inside of your nose.
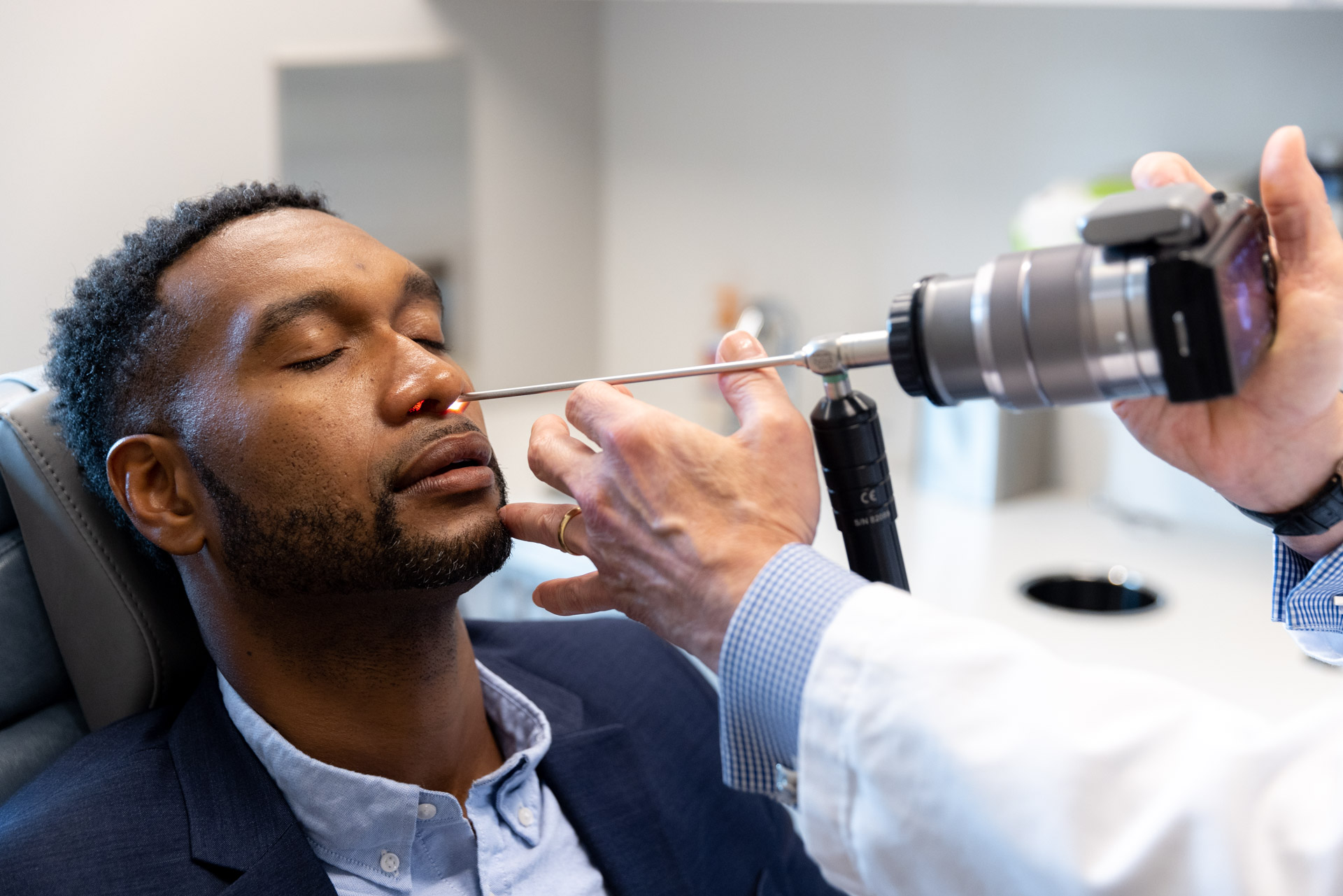
If your nose is congested or swollen turbinates are obscuring a full view of the inside of the nose, you can decongest your nose by using a medicated nasal spray to improve visibility. For a deeper inspection of the nasal cavity, openings of the sinuses and the back of the nasal airway, we can also use a flexible or rigid nasal endoscope.
While most deviated septums can be diagnosed by a thorough nasal examination, some may use CT scans to better visualize the back of the nose and the sinuses. If you have recurrent sinusitis, a CT scan will add more information on the status of your sinuses that can’t be seen, even with a nasal endoscope. Some insurance companies actually require or highly recommend a CT scan to further document a deviated septum.
Recently, our NYC offices have been using intra-nasal photographs taken with a nasal endoscopic camera to circumvent the need for a CT scan.

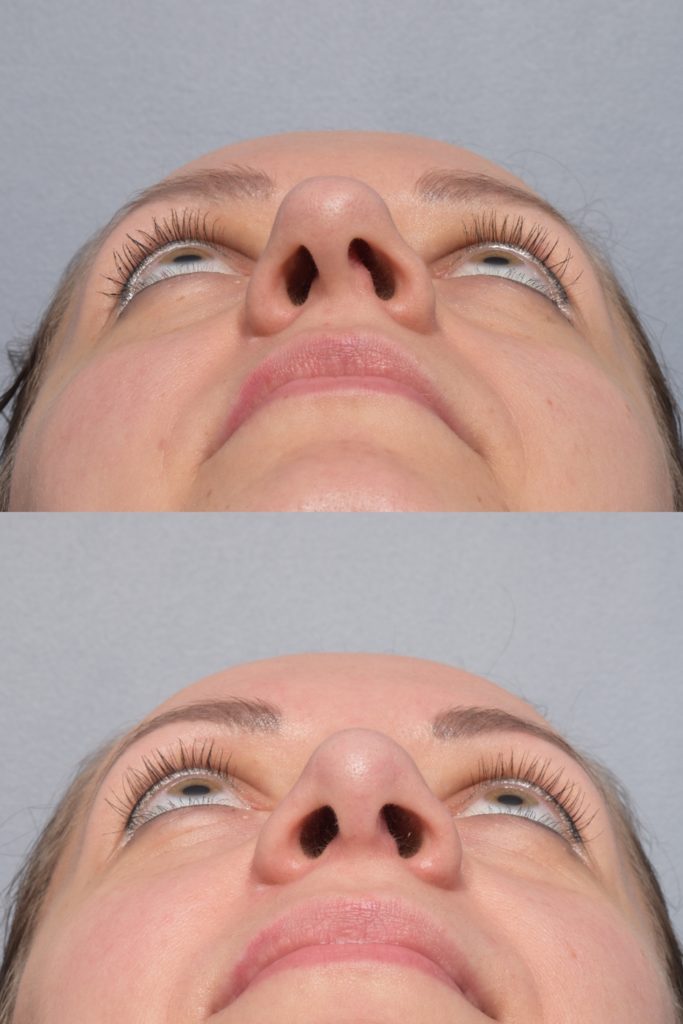
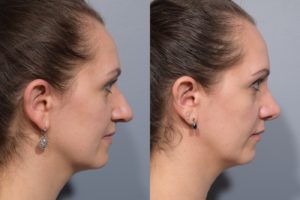
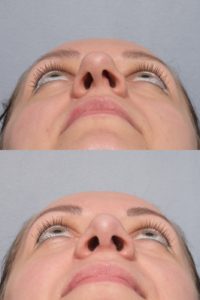
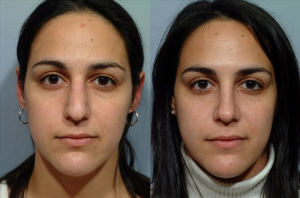
Fixing a deviated septum does not alter the appearance of your nose like cosmetic rhinoplasty because Dr. Pearlman leaves a strong support along the bridge and bottom of the nose. There also shouldn’t be any “black and blue” under the eyes or even an external cast necessary.
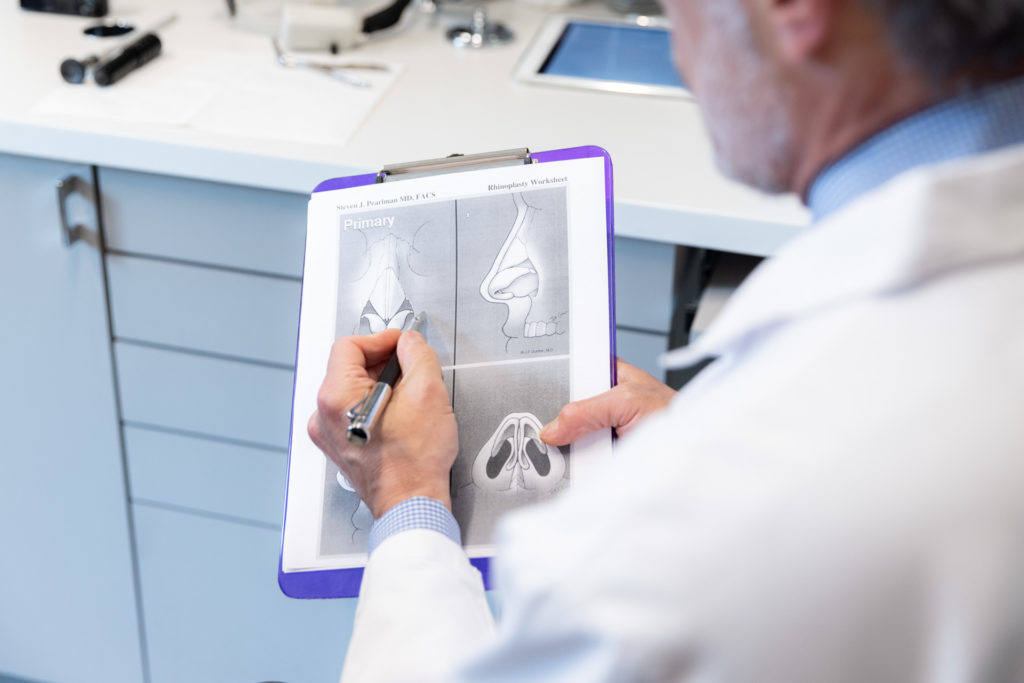
Septoplasty
Achieves: Functional nasal restoration (improves breathing)
Alters: The septum (the bone and cartilage separating the left and right airways in the nose)
Open or Closed Approach: Closed (endonasal)
Covered by Insurance: All or partial (depending on your insurance plan) Of course deductibles and co-insurance may apply.
Rhinoplasty
Achieves: Cosmetic improvement (enhances appearance)
Alters: The outer shape, size, and projection of the nose and/or nostrils
Open or Closed Approach: Open or closed
Covered by Insurance: Not generally
Combining the Two With a Septorhinoplasty
If you have a deviated septum and would like to improve the appearance of your nose, septoplasty and rhinoplasty can be performed together as one operation known as septorhinoplasty. Septoplasty is not an excuse to get a rhinoplasty, but is often part of the motivation if you are looking to improve the appearance of your nose as well.
Patients should be aware that most insurance companies do not cover fees for rhinoplasty, even when it is performed with a septoplasty.
Other Causes of Nasal Blockages
A deviated septum is not the only reason your nose could be continually feeling stuffed or blocked, and there are procedures to help these as well: turbinate surgery and functional endoscopic sinus surgery.
Sinus Surgery
The sinuses drain into the nose through tiny passages or corridors between the turbinates. When these small ports get blocked by a cold or allergies, the mucus backs up and bacteria can pool. This acts like a stagnant pond.
It then becomes a cycle of more bacteria, more toxins and more swelling. Antibiotics and sometimes nasal sprays and/or decongestants are necessary to sterilize the sinuses. Then they can drain better. However, if you have very tiny sinus openings, this cycle may keep on repeating, which is where an endoscopic sinus surgery can help. See the FAQ section to learn more about endoscopic sinus surgery.

Little Downtime
Since the majority of septoplasty surgeries are performed from the inside through a closed or endo nasal approach, there is much less recovery/downtime needed to heal from this procedure.
Dr. Pearlman typically tells all his septoplasty patients that their mother couldn’t tell they had anything done 2 days after surgery. Only in very extreme circumstances (less than 1 in many hundreds) does the nose need to be “opened” to correct an extremely deviated septum.

Breathe Easier
You deserve to have the best quality of life possible, and a deviated septum can have a negative impact by hindering your breathing, sleeping, and comfort. A septoplasty in NYC will give you the ability to breathe easily and comfortably. It can even improve pulmonary function in some patients.

Feel Better
Whether you realize it or not, a deviated septum can cause other health issues. While many people are used to struggling with the discomfort associated with this concern, you should not have to live with it. A septoplasty in NYC by Dr. Pearlman will help you feel fantastic.

Expertise
Dr. Pearlman is among the top New York’s nose surgery veterans as a Double Board-Certified Otolaryngologist (Ear, Nose and Throat doctor), and Facial and Reconstructive Plastic Surgeon. He uses his expertise to achieve significant improvement for his patients for life changing outcomes.

A Personal Consultation With Dr. Pearlman
How it Works
Full Nose Examination & Imaging
Ask Questions
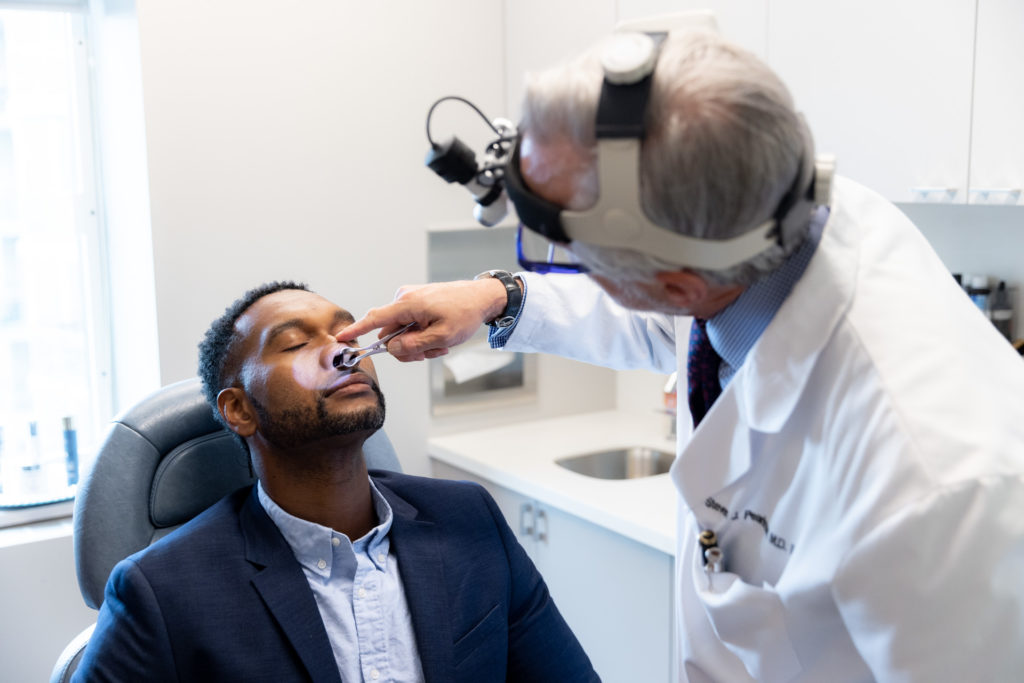
Based upon your unique nasal anatomy and intricacies of the nose Dr. Pearlman will perform a full examination of your nose inside and out to detect a deviated septum. This is to see if you are a candidate for septoplasty.
If you are interested in combining a rhinoplasty with your septoplasty (septorhinoplasty), he will then use advanced Mirror® 2D and Vectra® 3D imaging to demonstrate the potential changes to your nose to help you envision your future results.
The use of this technology is vital to understanding not only the potential changes and improvements to the nose itself, but also to visualize your new nose and how it balances with the rest of your facial features.
The right septoplasty surgeon for you should be able to provide a wealth of information regarding your procedure.
Throughout your septoplasty consultation at our NYC office, we highly encourage you to ask any and every question on your mind. We will walk you through every step of the process so you can feel confident in your decision to receive a septoplasty by Dr. Steven Pearlman.
Septoplasty Recovery
Dr. Pearlman and his staff will closely guide you through your post operative care.
What To Expect
He will provide detailed instructions on all aspects of the process to help guide your recovery from a septoplasty in NY.
The incision heals so that it is barely visible, if at all and only when viewed up close and from below the nose.
Dr. Pearlman often says “someone will have to be close enough to be able to count your nasal hairs to see this incision.”
Results to change your quality of life
A septoplasty in NYC can drastically improve your nasal functionality so that you can breathe more easily. You’ll enjoy a newfound quality of life from this functional surgery with expert care every step of the way from the team at Pearlman Aesthetic Surgery.
Dr. Pearlman is renowned for his commitment to nose procedures through decades of experience while sharing that knowledge with others through his lectures and publications.

Top Rated Facial Plastic Surgeon
Dr. Pearlman
Frequently Asked Questions
Septoplasty
Rhinoplasty Financing
How is endoscopic sinus surgery performed?
Endoscopic sinus surgery uses tiny surgical telescopes called endoscopes to explore inside the sinus openings. They can then be surgically enlarged to enhance fluid drainage from the sinuses and prevent backup of mucus and bacteria.
Surgery of the sinuses may be a simple opening of the sinus outflow tracts called the middle meatus, or more aggressive cleaning out of the sinuses depending on the extent of sinus disease. CT scans and correlation with the response to medical treatment will help determine how extensive sinus surgery needs to be.
Endoscopic sinus surgery is frequently performed at the same time as septoplasty since a deviated septum is often a significant contributing factor. It can also be safely done in conjunction with cosmetic rhinoplasty.
How will a rhinoplasty affect a deviated septum?
Every patient being considered for nasal surgery, even cosmetic rhinoplasty (commonly called a “nose job”) should have a thorough examination of the inside of the nose to check for a deviated septum. That’s because any nasal surgery could make a deviated septum more symptomatic and suddenly create nasal blockage.
Even a few millimeters of narrowing of the sidewalls of the nose that usually occurs with rhinoplasty could make this small deviation of the septum more important and now cause obstruction. This is based on the physics of Bernoulli’s Law pertaining to air flowing through a column.
So, if a deviated septum is present, it needs to be fixed, even if the patient came in for a cosmetic rhinoplasty. Otherwise there is the risk of creating a new problem. Some patients may not even realize that they have been breathing predominantly out of only one nostril until it’s pointed out at the time of examination. It is also astounding when patients come in for a revision rhinoplasty with breathing issues and report that their surgeon never even looked inside their nose because it was just a cosmetic rhinoplasty.
What are turbinates?
Other structures in the nose that also contribute to the nasal airway are called turbinates. There are three turbinates on each side of the nose: lower, middle and upper. They are curly bones that are also covered by mucosa.
The turbinates help channel the air we breathe along a direct path from the nostril to the back of the throat then down into our lungs; this is called laminar flow. The turbinates also swell to warm and humidify the air we breathe and as a reaction to colds and allergies.
You could be outside in cold, dry air, and by the time the air gets to your lungs it is 98% humidity and body temperature.
This is mostly a function of swelling of the turbinates. The turbinates also have a natural cycle where one side swells and 6 to 8 hours it alternates to the other side.
Sometimes you may cover one of your nostrils and the airflow is good, but when you switch, the other is less. This cycle will alternate sides. Rarely do people breathe fully through both nostrils at the same time.
The nasal cycle is also affected during sleep. The downhill nostril will swell by gravity and you breathe more through the uphill nostril. This is why when you turn over there is a brief wave of air you feel. It’s the uphill nostril opening up.
What is the anatomy of the nasal septum?
The nasal septum is the wall in the center of the nose that divides it into two sides. The front 2/3 is made of cartilage and the back portion is thin bone.
The septum, as well as the entire nasal cavity is lined by smooth shiny skin called mucosa that covers the cartilage and bone.
The septum sits on a small groove of bone called the maxillary crest that is the top of the bone that makes the palate (roof of the mouth). The septum extends from the floor of the nose to the bridge above and all the way down to the nasal tip below. If you put your finger in your nose and feel a wall in the middle, that’s your nasal septum.
What is the Nasal Valve and how is it improved?
Internal valve issues of excessive narrowing of the upper lateral cartilages after cosmetic rhinoplasty is one of the most common issues addressed in revision rhinoplasty. The treatment is the placement of grafts of your own cartilage to support that internal nasal valve, called spreader grafts.
These grafts are usually taken from nasal septal cartilage. Since we found that this issue was occurring so often, most rhinoplasty surgeons, including Dr. Pearlman, actually place spreader grafts in primary rhinoplasty to prevent internal valve issues in the first place in many patients.
The external nasal valve is lower down in the nose and comes from the strength and support of the nostrils by the tip cartilages called the lower lateral cartilages. The external nasal valve can be compromised or narrowed by a number of causes: too much cartilage is removed from the nasal tip during rhinoplasty, sutures used to narrow the nasal tip are too tight or the shape and position of the lower lateral cartilages are such that they don’t offer sufficient support for the nasal airway.
The treatment for a narrow nasal valve is common during revision rhinoplasty, or even preventing one in the first place during primary rhinoplasty is also by the use of cartilage grafts. These are called alar struts, spreader grafts or batten grafts.
What is the nasal valve?
The nasal valve is the narrowest part of the nose. It is actually divided into two parts: internal valve and external valve. When you have nasal obstruction, it is sometimes from nasal valve issues in addition to, or instead of, a deviated septum or enlarged nasal turbinates.
The internal nasal valve is in the middle third of the nose. The cartilages called the upper lateral cartilages insert into the nasal bones above and intersect with the top of the nasal septum in the midline.
If you run your finger down the side of your nose, you will likely feel a drop off below the top third of the nose. This is where the upper lateral cartilage is inserted under the nasal bone.
When a nasal hump is removed and the gap closed, the upper lateral cartilages may get even narrower.
What will the first week of recovery entail?
You will have some bruising and swelling around the eyes during the first week of recovery. Some patients need time to adjust to breathing through their mouth; it’s akin to having a mild cold. Fatigue from the anesthesia is common for the first day or two. Patients should rest the first few days in an upright position to minimize swelling for better healing.
Will a septoplasty alter the way my nose looks?
Septoplasty alone has no effect on the appearance of your nose. There is no external splint or cast. Some patients choose to have cosmetic surgery at the same time. If you choose to, you may have a combination of a septoplasty and rhinoplasty (septorhinoplasty) to alter the way your nose looks along with breathing functionality.
Will a septoplasty improve my breathing forever?
Septoplasty will long lastingly straighten a deviated septum. However, nasal obstruction may also be due to other anatomic and functional issues. For most patients, they experience long lasting improvement in breathing.
Will insurance cover a septoplasty in NYC?
If you have blockage of your breathing and documented treatment for nasal obstruction, insurance can often cover septoplasty surgery. This will be only for the functional procedure of septoplasty, not rhinoplasty.
Patient
Experiences

Persistent in the Pursuit of Perfection
For decades, Dr. Pearlman has been persistent in his search for perfection as the best septoplasty surgeon in New York. He brings evolution, experience, expertise, and uniqueness to his septoplasty patients in our Park Avenue office. The goal of Pearlman Aesthetic Surgery is to help patients to actualize their ideal self-image for the highest level of personal authenticity and attractiveness possible. Dr. Pearlman couples an attentive bedside manner and genuine concern for his patients’ welfare to deliver the best septoplasty results.

Learn if you're a candidate for septoplasty in NYC
Our virtual rhinoplasty consultation tool will help you learn more about the possibilities for your septoplasty procedure.
Request Appointment
Address
110 E 60th ST #908 New York, NY 10022
Hours
Monday
9 am – 5 pm
Tuesday
9 am – 5 pm
Wednesday
10 am – 6 pm
Thursday
9 am – 5 pm
Friday
9 am – 5 pm
Sat - Sun
closed